Your biology, doing the rebuilding.
PRP Facial uses concentrated platelets from your own blood to trigger the skin's collagen-production machinery — producing real, progressive improvements in skin quality, firmness, and radiance over 4–6 weeks.
PRP doesn't treat surface symptoms. It stimulates the biology that creates them.
Growth factors in your own blood trigger fibroblast activity — the cells that produce collagen, elastin, and the structural proteins that determine skin quality. The result builds over weeks, not days.
The progressive loss of collagen and elastin from the late 20s onward produces the characteristic softening of facial skin. PRP growth factors (PDGF, TGF-β, EGF) directly stimulate the fibroblasts responsible for producing new collagen and elastin — producing a genuine increase in dermal density over 4–12 weeks. Loss of cheek volume — where the face begins to look hollow or deflated — is one of the primary signs of facial aging that PRP's collagen restoration addresses progressively over the treatment series.
Patients who've done multiple HydraFacials and peels and still have chronic dullness often respond significantly to PRP because the growth factors reach the dermal layer where the underlying issue resides. Improved vascularization from PRP-stimulated angiogenesis also produces a lasting improvement in skin radiance.
Fine lines that have a textural component — not just dynamic expression lines — respond to PRP's collagen-stimulating effect. The new collagen produced over 6–12 weeks plumps and smooths the dermis from beneath, reducing fine line appearance and improving overall skin quality. Fine expression lines including crow's feet around the eyes and perioral lines around the mouth respond well to the collagen-stimulating effect of PRP — areas where the skin is thin and dynamic movement accelerates fine line formation.
PRP applied to the periorbital area improves the thin, delicate skin under the eyes — reducing crepiness, stimulating collagen in the tear trough area, and improving the dark circle appearance caused by skin thinning rather than pigmentation. One of the most impactful applications of PRP in facial aesthetics.
PRP delivered via microneedling across acne-scarred skin stimulates the collagen remodeling needed to improve shallow to moderate textural scarring. Most effective for rolling scars and shallow icepick scars — produces best results when combined with a surface treatment protocol.
PRP Facial is an excellent maintenance treatment for patients who've had PDO threads, fillers, or Botox — stimulating ongoing collagen production that extends and deepens the results of structural treatments. Commonly used 2–3 times per year as part of a comprehensive aesthetic maintenance protocol.
If your skin concern is quality — firmness, radiance, texture — PRP addresses the biology behind it.
Surface treatments improve what's on the skin. PRP improves what produces it — the dermal layer where collagen and elastin are made. That's a fundamentally different category of intervention.
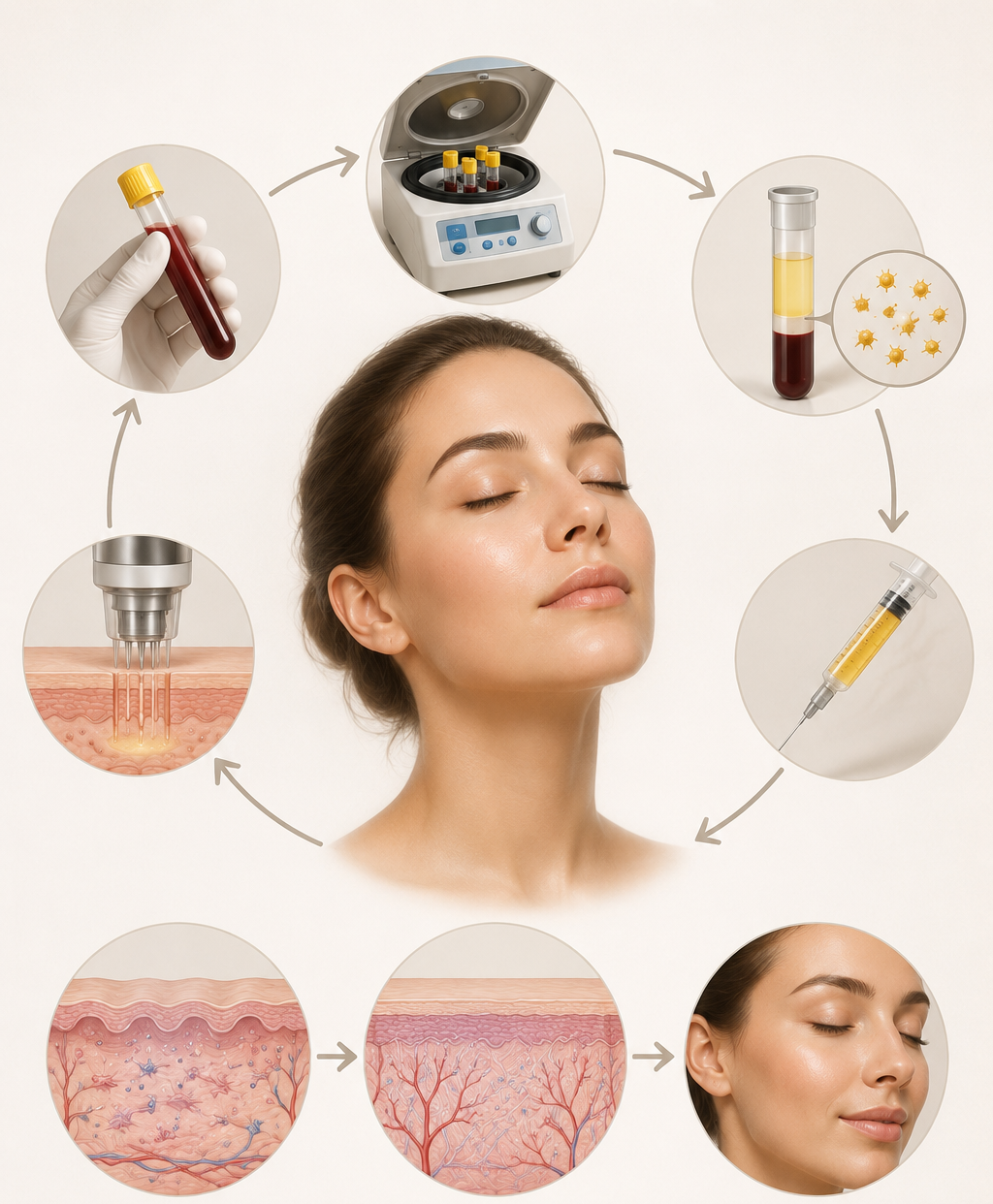
Your platelets already know how to heal skin.
Platelets are the cells responsible for initiating the healing response whenever tissue is damaged. They contain growth factors — PDGF, TGF-β, EGF, VEGF, IGF-1 — that signal fibroblasts to produce collagen, stimulate new blood vessel formation, and initiate cellular repair. PRP (Platelet-Rich Plasma) concentrates these platelets from your own blood to 3–5x their normal density and applies them where skin regeneration is needed.
The procedure begins with a small blood draw — comparable in volume to a standard blood test. Your blood is centrifuged for 10–15 minutes, separating the platelet-rich plasma from red blood cells. The resulting PRP is then applied to the face via microneedling — creating micro-channels that allow deep penetration of the growth factors into the dermis — or injected directly into specific areas for targeted treatment.
Results develop progressively over 4–6 weeks as the growth factors stimulate new collagen production in the treated tissue. The full effect is typically visible at 3 months, when the new collagen has had time to organize and mature. Most patients notice a visible improvement in skin thickness, radiance, and firmness. A series of 3 monthly treatments produces the most significant and durable results — with annual maintenance to sustain the baseline improvement.
Medical history for platelet function disorders or anticoagulant medications (both contraindications). Active skin infections or inflammatory conditions in the treatment area. Prior treatment history — PRP works well alongside and after other modalities. Your goals: PRP for quality improvement vs. PRP specifically for under-eyes or texture requires slightly different application protocols. Your physician designs the approach accordingly.
PRP stimulates real structural tissue change.
Unlike topical treatments that sit on the skin's surface, PRP growth factors penetrate to the dermal layer and produce measurable increases in collagen density, elastin fiber organization, and vascular density over 6–12 weeks. The evidence base for aesthetic PRP has grown substantially over the past decade.
From a blood draw to better skin.
We assess your skin quality concerns, review your medical history for contraindications, and design your PRP protocol — number of sessions, application method (microneedling vs. injection), and combination with other treatments.
A small blood draw in our clinical setting — similar to a standard lab test. Your blood is centrifuged for 10–15 minutes to separate and concentrate the platelet-rich plasma. The entire preparation takes place before your eyes.
PRP is applied via microneedling for broad skin quality improvement, or injected directly for targeted areas (under-eyes, jawline, specific texture zones). 45–60 minutes total including prep. Mild redness for 24–48 hours.
3 monthly treatments produce the most significant results. Full effect visible at 3 months. Annual maintenance session sustains the collagen baseline. Many patients combine with PRF for enhanced depth and duration.
Medicine that
gets you.
PRP outcomes depend on preparation quality, platelet concentration, and application technique. Our physicians are trained in the clinical protocols that produce consistent, measurable results.
Your Own Biology — No Foreign Material
PRP uses your own platelets. There is no risk of allergic reaction, immune rejection, or transmission of external pathogens. The growth factors are identical to those your skin would produce in response to tissue damage — just at a therapeutic concentration.
Precise Centrifuge Protocol
PRP quality depends entirely on the centrifuge speed and time used during preparation. We follow validated protocols that produce consistently high platelet concentrations — not a variable result from an imprecise preparation.
Application Method Matched to Concern
Microneedling-delivered PRP for broad skin quality, direct injection for targeted areas (tear troughs, textural scarring, jawline). The application method changes the therapeutic depth and mechanism — we select it based on your specific goals.
Combination Strategy
PRP is most powerful as part of a planned treatment sequence — following a HydraFacial series that has primed the surface, or in combination with PRF for deeper collagen remodeling. We design the protocol around your complete aesthetic goals, not a single treatment.
Real patients.
Real results.
Everything you
want to know.
Your skin can rebuild.
Give it what it needs.
A free consultation and a clear assessment of what PRP can realistically achieve for your skin. A protocol designed around your biology and goals — not a standard package.