Your own platelets. Your own healing. Accelerated.
Platelet-Rich Plasma (PRP) therapy injects concentrated platelets from your own blood into injured tissue — delivering natural cytokines, stem cells, and bioactive growth factors that boost healing in tendons, joints, and ligaments. Used by Tiger Woods, Hines Ward, and professional athletes worldwide.
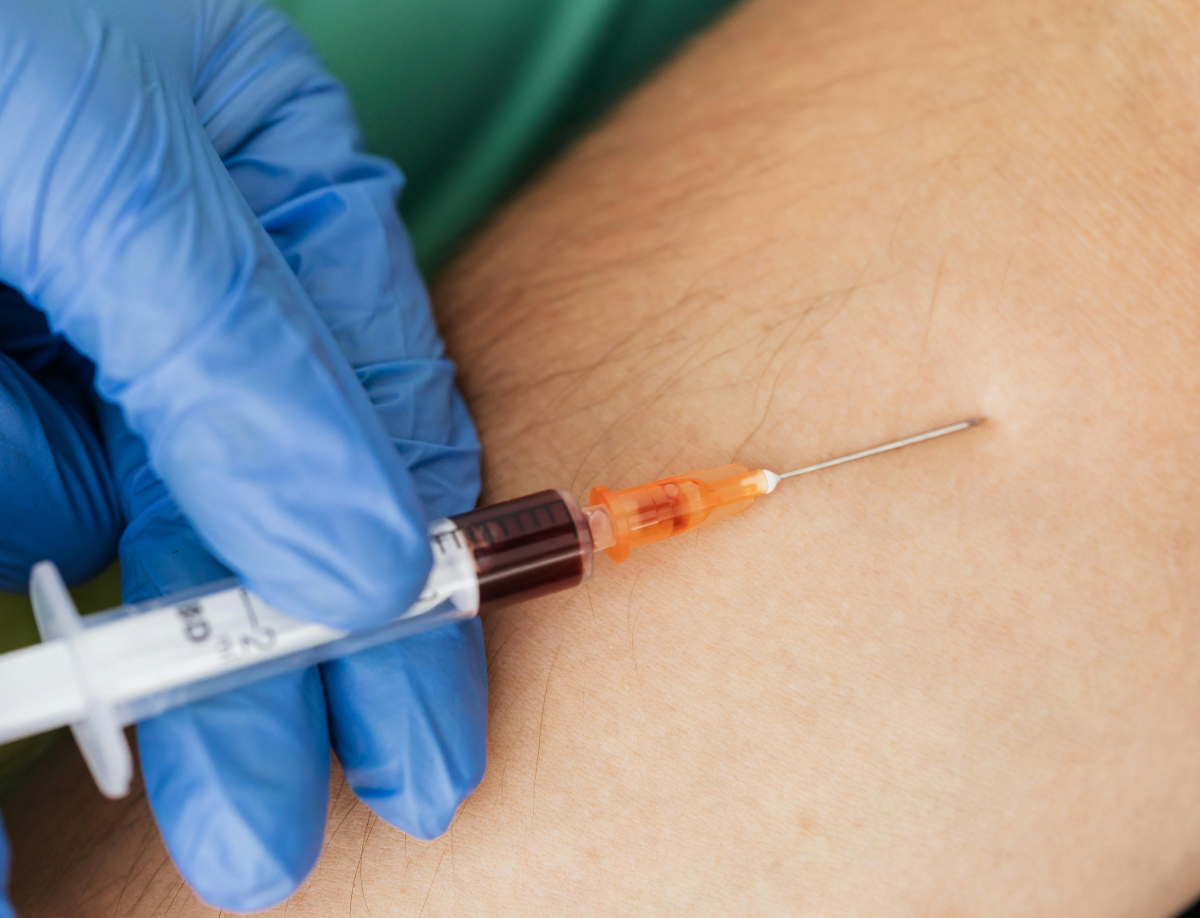
From arthritis to rotator cuff — PRP addresses what conventional treatment can't.
PRP injections have been used in orthopedic treatments since the early 2000s. They deliver the body's own growth factors directly to injured tissue — stimulating repair processes that rest, medication, and physiotherapy alone cannot activate.
Professional athletes including Tiger Woods, Hines Ward, and Cliff Lee have used PRP treatment to speed up recovery from injuries. Tennis elbow, torn ligaments, and rotator cuff injuries — conditions that often require surgery or produce incomplete healing with rest alone — respond to PRP's concentrated growth factors, which directly stimulate the tissue repair processes that chronic or complex injuries have failed to complete.
Runner's knee (patellofemoral syndrome), tendonitis, and plantar fasciitis are among the most treatment-resistant overuse injuries. PRP injections deliver bioactive proteins including fibronectin, vitronectin, and fibrin — along with growth factors that stimulate cell replication and vascular endothelial growth — directly into the damaged tendon or fascia where healing has stalled.
PRP is an excellent alternative therapy that helps decrease osteoarthritis symptoms — reducing pain and inflammation while stimulating cartilage and synovial tissue repair. Used for both knee and hip osteoarthritis in patients who want to delay or avoid joint replacement surgery, PRP injections into the joint space deliver concentrated growth factors that conventional arthritis medications don't provide.
Office workers and active patients with consistent neck, shoulder, and lower back pain can benefit from PRP therapy directed at the affected spinal structures — discs, facet joints, and surrounding soft tissue. PRP's collagen-stimulating effect and anti-inflammatory growth factors address the structural component of chronic spinal pain.
Common hand injuries and repetitive strain conditions — carpal tunnel, trigger finger, De Quervain's tenosynovitis — respond to PRP injection. Office workers experiencing consistent hand, wrist, and forearm pain from repetitive computer use represent a large proportion of PRP patients. The growth factors stimulate tendon and ligament repair in ways that rest alone cannot achieve.
PRP is particularly effective for injuries and pain conditions that have been unresponsive to conventional treatment. Where rest, physiotherapy, cortisone injections, and medications have failed to produce lasting improvement, PRP's concentrated biological stimulus often succeeds — because it addresses the repair mechanism directly rather than managing inflammation.
If your injury hasn't healed the way it should, PRP gives your body the biological tools it was missing.
PRP is taken from your own blood — there is no risk of allergic reaction or rejection. It is used for sports injuries, arthritis, chronic pain, and joint deterioration. Schedule an appointment to find out if PRP treatment is right for your specific condition.
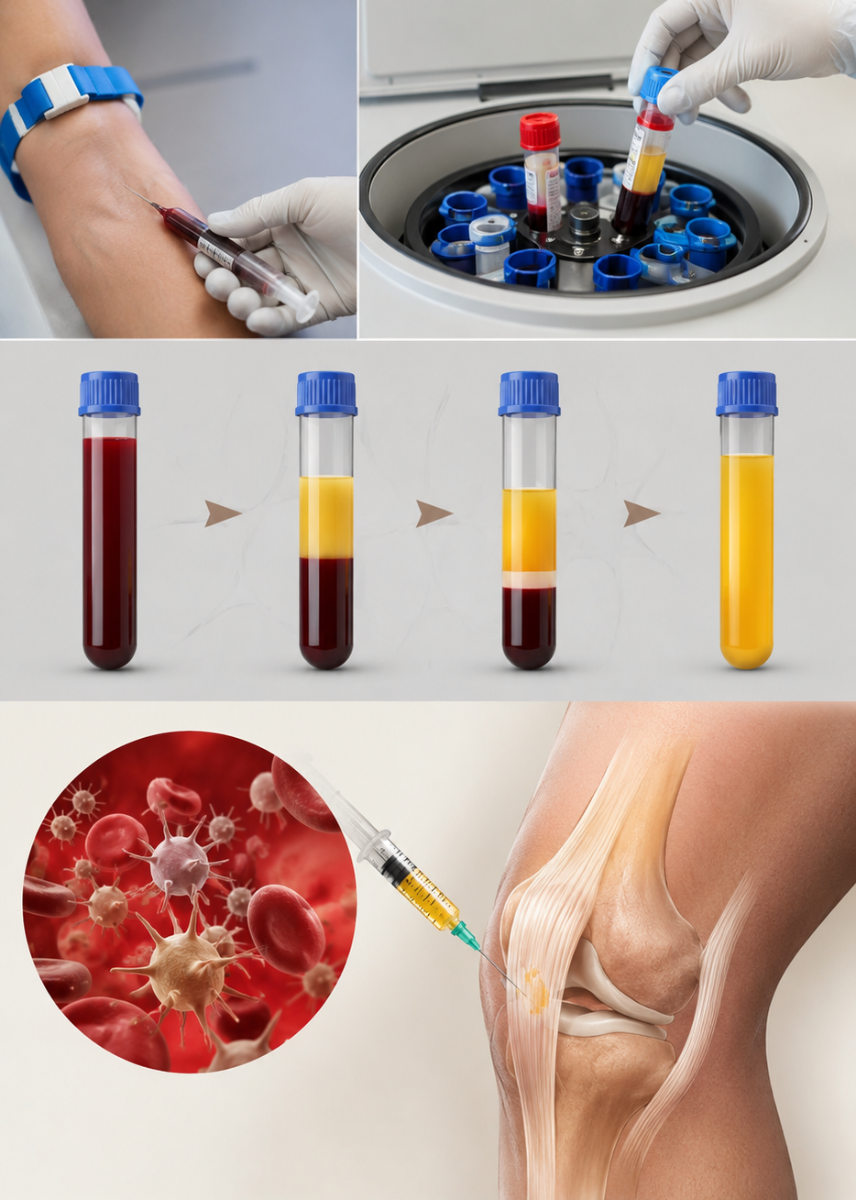
Concentrated platelets. Concentrated healing.
Platelet-Rich Plasma (PRP) is derived from a patient's own blood. A blood sample is drawn and centrifuged to separate and concentrate the platelet-rich plasma — which differs from ordinary blood in that it contains higher concentrations of platelets and cell ratios with bioactive factors that boost natural wound healing. The resulting PRP is then injected directly into the damaged area — tendons, joints, ligaments — where it delivers its therapeutic payload.
The mechanism is multi-layered. PRP injections supply injured areas with natural cytokines, stem cells, and bioactive growth factors that directly boost healing. They also lead to local inflammation and wound healing mediated by bioactive proteins — including plasma proteins fibronectin, vitronectin, and fibrin — that form the structural scaffold for new tissue. Research shows PRP stimulates cell replication, vascular endothelial growth, proliferation of myoblasts, and insulin-like growth factor-1 (IGF-1) that repairs muscular and skeletal structures.
New collagen gradually tightens the damaged area, making it stronger over weeks and months. The result is genuine tissue repair — not just pain management. For injuries that have been unresponsive to conventional treatment, PRP often produces the structural improvement that rest and rehabilitation alone could not achieve.
Natural cytokines · Bioactive growth factors · Plasma proteins (fibronectin, vitronectin, fibrin) · IGF-1 (insulin-like growth factor — repairs muscular and skeletal structures) · Stimulation of cell replication and myoblast proliferation · Vascular endothelial growth factor (new blood vessel formation). All from your own blood — no foreign material, no rejection risk.
Used by professional athletes. Backed by orthopedic research.
PRP has been used in orthopedic medicine since the early 2000s — with professional athletes including Tiger Woods and Hines Ward among its most visible proponents. The evidence base for sports injuries, tendinopathy, and osteoarthritis is well-established.
From injury that won't heal to tissue that's actually repaired.
We assess your specific injury, its duration, what treatments you've already tried, and whether PRP is the right intervention. We'll be direct about what PRP can and can't achieve for your specific condition.
Small blood draw in our clinical setting. Centrifuged to concentrate platelets to 3–5x normal blood levels. The PRP is prepared in-clinic and ready for injection within 15 minutes.
PRP injected directly into the damaged area — tendon, joint, ligament, or soft tissue. Ultrasound guidance used for precision when appropriate. Mild soreness for 2–5 days post-injection as the inflammatory healing response is triggered.
Healing develops over 4–12 weeks as new collagen forms and tissue strengthens. Follow-up at 6 weeks to assess response. Most injuries require 1–3 PRP sessions. Complex conditions may benefit from combining with shockwave therapy.
Medicine that
gets you.
PRP is only as good as the preparation quality and injection precision. We use validated centrifuge protocols and physician-level injection technique for every session.
Your Own Biology — No Risk of Rejection
PRP is entirely autologous — drawn from your own blood. There is no risk of allergic reaction, immune rejection, or infection from an external source. The growth factors are identical to those your tissue would produce in response to injury — just at concentrated therapeutic doses.
Validated Centrifuge Protocol
PRP quality depends entirely on the centrifuge speed and preparation method. We follow protocols that produce consistently high platelet concentrations — ensuring the product injected is therapeutically potent.
Precise Injection Technique
PRP injected into the wrong tissue plane or at insufficient depth produces inferior results. Our physicians use precise anatomical knowledge and ultrasound guidance where appropriate to ensure the growth factors reach exactly where they need to.
Combined With Shockwave When Appropriate
For many musculoskeletal conditions, combining shockwave therapy (mechanical stimulus) with PRP (biological growth factors) produces significantly better outcomes than either alone. We design combination protocols where the clinical evidence supports it.
Injuries that finally
healed properly.
Everything you
want to know.
Set yourself free
from pain and injuries.
A free consultation and assessment of your injury or chronic pain condition. We'll determine whether PRP, shockwave, or a combination is the right approach — and give you honest expectations for recovery timeline.